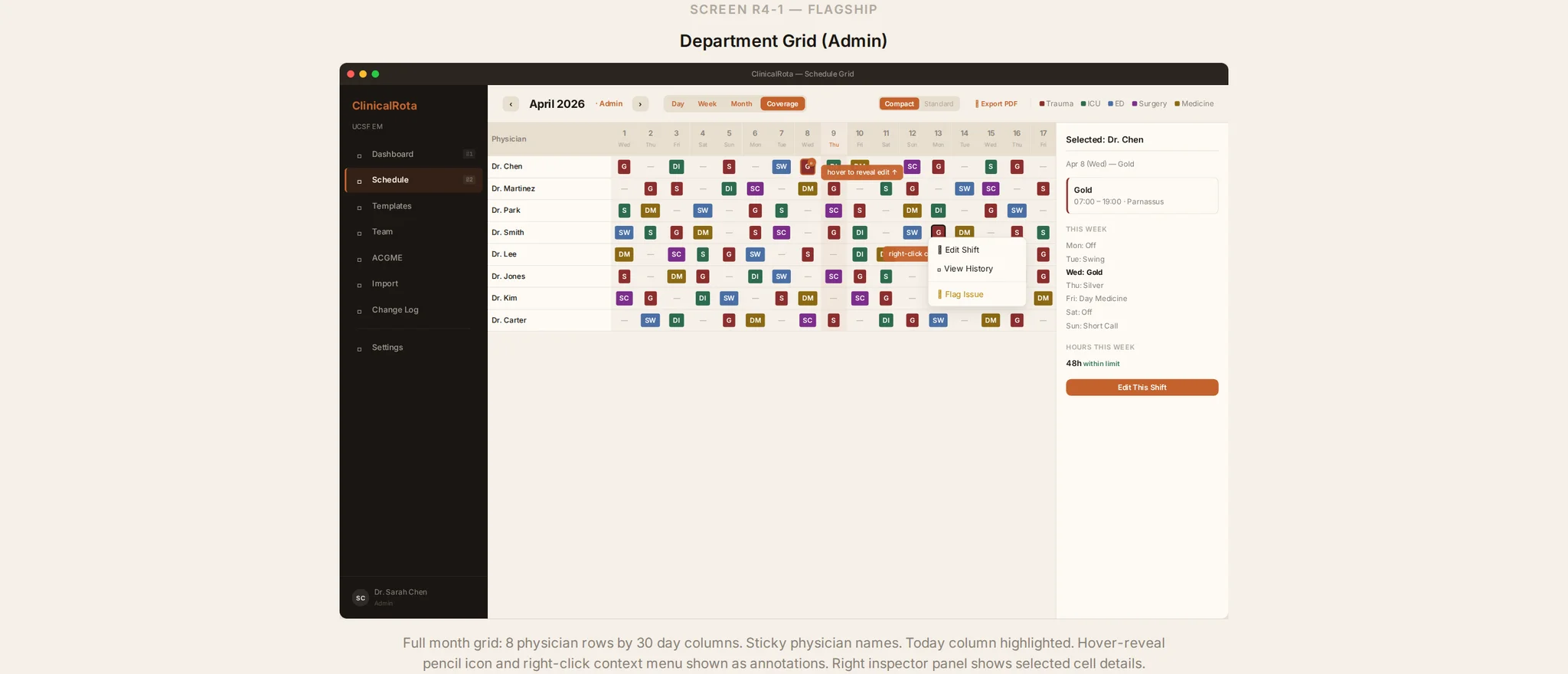
Why On-Call Scheduling Deserves More Attention Than It Gets
Ask a hospital administrator what keeps them up at night, and on-call scheduling will appear on that list far more often than it should. Not because it is the most clinically complex challenge a department faces, but because it is relentlessly difficult to do well with the tools most hospitals still use.
On-call scheduling sits at the intersection of patient safety, labor law compliance, staff wellbeing, and operational continuity. Get it right and your department runs smoothly, your clinicians feel respected, and your coverage gaps are rare. Get it wrong and you are managing the consequences for weeks: last-minute scrambles to fill uncovered shifts, frustrated physicians who feel the rotation is unfair, overtime costs that erode your department’s budget, and staff turnover that costs the organization far more than a better scheduling process ever would.
Most departments manage on-call scheduling with a combination of spreadsheets, institutional memory, and escalating levels of manual effort as complexity increases. This guide is for the administrators and clinical operations leaders who are ready to do it better.
Understanding What Makes On-Call Scheduling Hard
On-call scheduling is more complex than standard shift scheduling for several reasons, and it is worth naming them explicitly before discussing solutions.
Variable call burden is inherently unequal. Not all on-call shifts are created equal. A Friday night call in an emergency department carries a fundamentally different workload than a Tuesday on-call in an outpatient specialty department. If your scheduling system treats these as equivalent, your physicians will know it, and they will be right to feel that the distribution is unfair.
Coverage requirements are multidimensional. You are not just filling time slots. You are matching credentialed, qualified clinicians to coverage responsibilities that may require specific training, hospital privileges, or scope of practice authorizations. An on-call physician who cannot perform the procedures that will most likely be needed during their shift is not a valid solution to a coverage gap.
Personal constraints are numerous and legitimate. Physicians have second jobs at other facilities, academic commitments, family obligations, and leave requests that all interact with the schedule in complex ways. Capturing these constraints accurately and honoring them consistently while still meeting coverage requirements is a combinatorial problem that spreadsheets genuinely cannot solve at scale.
Schedules change constantly. Sick calls, leave requests, credentialing updates, and shift swaps all pull a published on-call schedule away from reality almost immediately. Without a system that can handle amendments cleanly and propagate notifications automatically, administrators spend enormous amounts of time managing change rather than managing the department.
Equity requires active enforcement. Fairness in on-call distribution does not happen automatically. Without explicit rules that limit how many undesirable shifts any single physician can be assigned within a period, the path of least resistance is to lean on whoever is most available or least likely to push back. This creates resentment, and eventually attrition.
Core Principles of Effective On-Call Scheduling
Regardless of the tools you use or the specialty of your department, effective on-call scheduling rests on a small number of principles that hold universally.
Encode your rules, do not rely on memory
Every department has scheduling rules. Some are formal (ACGME duty-hour limits for residents, labor law restrictions on consecutive hours), and some are informal conventions that have developed over time. The informal rules are the dangerous ones, because they exist only in the heads of whoever has been building the schedule longest.
When that person leaves, goes on leave, or simply has a bad month, gaps in institutional knowledge start to show. Disputes arise because different people remember the rules differently. Exceptions that were granted as one-time accommodations get locked into the schedule as permanent entitlements.
The solution is to document every scheduling rule explicitly and enforce it through your scheduling process. This does not mean building a giant policy document that no one reads. It means encoding rules in a format your scheduling system can apply automatically. Which clinicians are qualified for which coverage responsibilities. Maximum consecutive on-call days. Minimum rest periods between call shifts. Holiday rotation formulas. These should be defined once and applied consistently, not reconstructed from memory each cycle.
Collect preference data early and systematically
The biggest source of scheduling conflict is the gap between what clinicians expect and what the schedule delivers. The single most effective intervention in closing that gap is to collect preference data, including availability, time-off requests, shift preferences, and swap requests, well in advance of the scheduling period through a structured process that creates a clear record.
Email threads, paper forms, and verbal agreements are not structured processes. They create ambiguity, lose information, and make it impossible to document whether a request was received and considered. A systematic preference collection process, ideally through an online interface that timestamps every submission and creates a clear record of what was requested and what was accommodated, protects both the clinician and the administrator.
Collecting preferences early also gives schedulers time to identify conflicts before the schedule is published. A physician who submitted a vacation request for the same week as a mandatory coverage event six weeks in advance is a solvable problem. The same conflict discovered two days before the schedule goes live is a crisis.
Distribute undesirable shifts explicitly and transparently
Every department has shifts that no one wants. Nights. Weekends. Holiday weekends. Call on major holidays. These shifts need to be covered, and they need to be distributed fairly. That means the distribution criteria need to be explicit and visible to every member of the team.
What does fair mean in practice? It depends on the department and the team, but the common elements are: everyone covers their share of undesirable shifts within each scheduling period; no one is assigned more than a defined maximum of consecutive or monthly undesirable shifts; and the historical distribution is accessible so that anyone who thinks they are carrying an unfair share can verify it rather than just suspect it.
Transparency about distribution is as important as the distribution itself. When clinicians can see how the schedule was built and what rules it follows, complaints about fairness shift from subjective grievance to verifiable question. Either the rules were applied correctly, or they were not, and both outcomes are resolvable.
Plan for change before it happens
On-call schedules are disrupted constantly. The question is not whether disruptions will occur. It is whether your process for handling them is organized or chaotic.
A resilient on-call scheduling process has three elements: a mechanism for clinicians to request shift swaps directly with one another instead of routing every change through an administrator; a clear escalation path for coverage gaps that cannot be resolved by a swap; and a communication system that notifies affected parties automatically when a change is made rather than relying on the administrator to contact everyone manually.
The shift swap piece is worth emphasizing. Many departments require administrator approval for every swap, which creates a bottleneck. A better approach is to allow physician-initiated swaps for shifts of equivalent on-call burden, subject to automated validation that both parties are qualified for the coverage responsibility, with administrator notification but not approval required. This reduces the administrative burden while maintaining appropriate oversight.
Common Failure Patterns
Understanding what goes wrong in on-call scheduling is as useful as knowing what to do right. These are the patterns that appear most consistently in departments that are struggling.
The spreadsheet that only one person understands. This is the single most common and most dangerous failure mode. When the master on-call spreadsheet is maintained by one administrator and exists only in their local files, the department is one sick day away from a scheduling crisis. The knowledge is not institutional. It is personal. Departments in this situation are not just inefficient; they are fragile.
The rule that exists but is not enforced. The department has a policy limiting physicians to four on-call weekends per quarter. But when coverage gets tight, exceptions are granted informally, the exceptions compound over time, and eventually the rule exists only on paper. The physicians who pushed back on the exceptions feel vindicated; the ones who accepted them feel exploited. Trust erodes in both directions.
The preference process that is not a process. Requests come in through email, text, and hallway conversations over a two-week window with no clear deadline. Some are recorded in the spreadsheet; some are not. The schedule is published, and three physicians are immediately upset because their requests were not honored, or were not received. Whether the administrator is responsible for the failure or not, they bear the consequence.
The schedule that cannot absorb change. The schedule is published four weeks in advance with high-resolution detail. A physician develops a family emergency two weeks in. The only mechanism for a swap is to email the administrator, who emails the entire group asking if anyone can cover, waits two days for responses, and then manually updates the spreadsheet and re-notifies everyone. This is not a scheduling system. It is a calendar with extra steps.
What Modern Scheduling Systems Do Differently
The operational problems described above are not new, and the solutions are increasingly well-understood. Modern scheduling platforms, purpose-built for healthcare rather than adapted from generic workforce management software, address the core failure points in a few specific ways.
Constraint-based scheduling means that coverage rules, qualification requirements, and fairness parameters are encoded in the system and enforced automatically rather than checked manually. A scheduler building the on-call roster for next month does not need to remember that Dr. Chen cannot be assigned to Level 1 trauma call because her hospital privileges lapse next quarter. The system flags it. The manual cognitive load of compliance checking is offloaded to the software.
Self-service preference collection means that physicians submit their availability and requests through an online interface with a clear deadline and an immediate confirmation. The administrator sees a structured record of every submission. There is no ambiguity about what was requested or when, and the system can surface conflicts before the schedule is built rather than after it is published.
Algorithmic schedule generation means that the system evaluates the full combination of constraints, preferences, and fairness parameters simultaneously and produces an optimized schedule rather than a manually assembled one. This is not about removing human judgment from the process. It is about letting the algorithm handle the combinatorial problem so that human judgment can focus on the tradeoffs that actually require professional assessment.
Real-time change management means that swap requests, coverage gaps, and last-minute changes are processed through the same system that holds the schedule, with automated validation and notification. An administrator who receives a sick call at 6 AM can identify qualified available physicians in the system, send an availability inquiry, and confirm a replacement before the morning huddle.
Making the Case for a Better Process
Administrators who know their current process is broken often face an internal challenge: how do you make the case for change to department leadership that has tolerated the status quo for years?
The most effective arguments are concrete and quantifiable.
Start with time. Track how many hours per scheduling cycle are spent building the schedule, handling preference requests, managing swaps, and resolving disputes. For many departments running on manual processes, the total easily reaches dozens of hours per cycle, time that comes directly out of the administrator’s capacity for everything else. Present that number with a dollar value attached.
Add overtime cost. Manual scheduling that cannot optimize for coverage efficiency tends to produce more overtime than necessary. If you can pull six months of overtime data and correlate it with scheduling patterns, you have a compelling anchor for the conversation.
Include turnover risk. Physician turnover in hospital-employed groups is expensive, often running well into the hundreds of thousands of dollars per departure once you account for recruiting, onboarding, and productivity ramp-up. Scheduling dissatisfaction is one of the most consistently cited factors in voluntary departures. If your department has had turnover conversations where scheduling fairness was a theme, document it.
Finally, be specific about what better looks like. Not “we need a new system” but “we need a system that can enforce our coverage rules automatically, collect preferences through a structured interface with a clear deadline, generate an optimized schedule that an administrator can review and publish, and handle swap requests without requiring administrator approval for every transaction.” That is a specification, not a wish list, and it gives leadership something concrete to evaluate.
The Standard Worth Holding Yourself To
On-call scheduling is one of those operational areas where the gap between mediocre and excellent is visible every day to the people it affects most. Physicians who feel the schedule is fair, flexible, and responsive to their input are more engaged, more satisfied, and more likely to stay. Administrators who have a scheduling process that actually works have the capacity to focus on the clinical and operational challenges that genuinely require their judgment.
The tools to close that gap are available, increasingly affordable, and proven at healthcare organizations that once faced the same problems you are facing now. The question is not whether better is possible. It is whether the current cost of staying with the status quo, in time, money, and staff wellbeing, has become high enough to justify making the change.
For most departments, it already has.
Clinical Rota is built specifically for healthcare scheduling: AI-powered schedule generation, structured preference collection, and real-time change handling without the administrative scramble. Book a demo to see how it handles your department’s specific constraints.