Healthcare scheduling software has a strange property. The people who depend on it most are often the people it was least designed for.
Schedulers learn to tolerate that. Physicians and nurses usually do not. They just work around it.
Why The Problem Persists
A lot of hospital software survives by being just good enough for the person administrating it.
The day-to-day users pay the price. They check multiple systems. They text each other to confirm changes. They memorize side rules. They rely on a chief resident, coordinator, or manager to translate the official schedule into the real one.
That is the pattern we kept seeing.
The Real Failure Mode
The problem is not only that building schedules is hard. It is that once a schedule exists, it is still hard to understand.
Who is on right now? Who changed this shift? Is the month fair? What happens if one person calls out? Which part of the schedule is thin and which part only looks full?
Those are basic questions. A surprising amount of current software answers them badly.
What We Built Instead
Clinical Rota started with concrete screens instead of a product claim because we did not want to bluff our way past the hard part.
The hard part is figuring out which pain is most real. Is it generation? Is it viewing? Is it compliance visibility? Is it coverage changes? Is it fairness? Different departments will answer that differently.
So instead of pretending to already know, we built screens that make the conversation concrete.
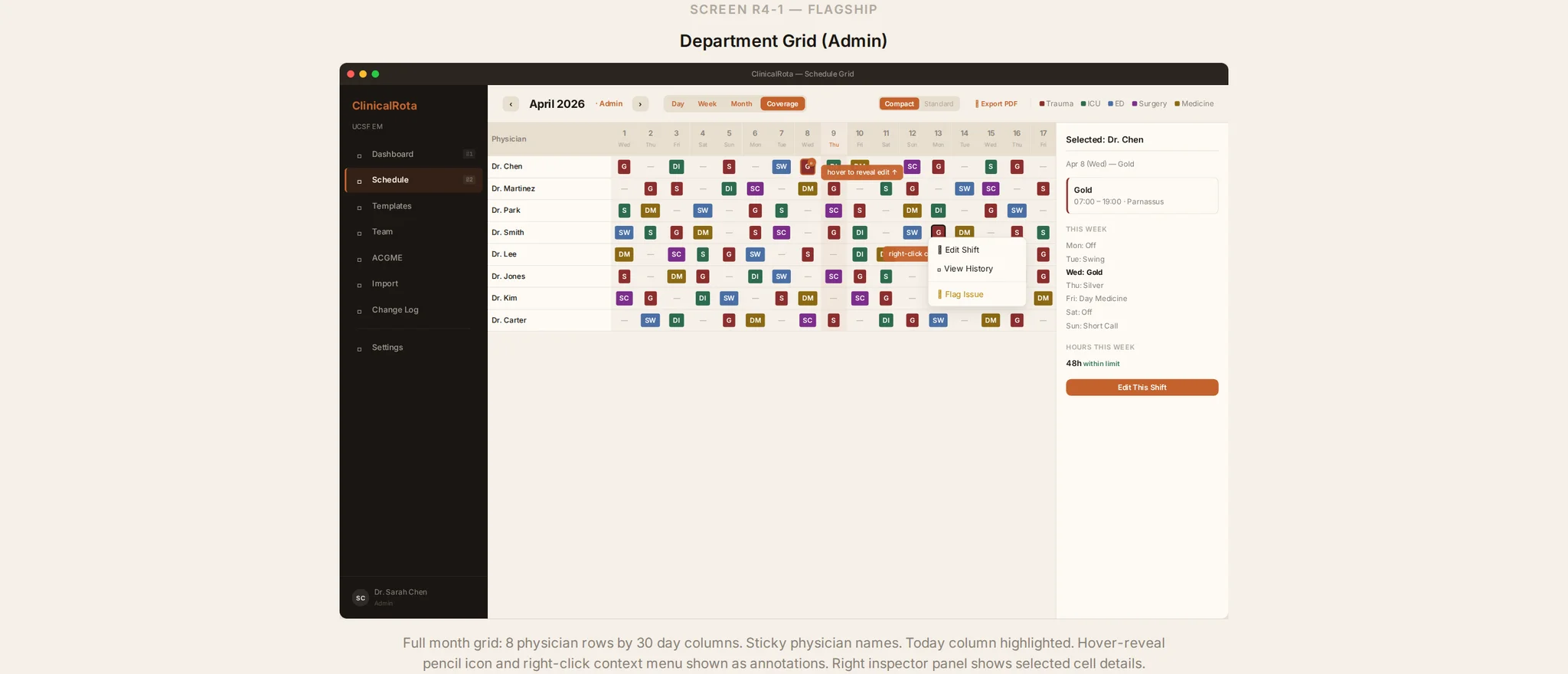
Why Start With Screens
The screens are not there to impress people with polish. They are there to force specificity.
A coordinator can point at a screen and say, “This part matters, this part doesn’t, and this is the real workflow you are missing.” A resident can say, “I would actually open this view,” or, “No, the thing I need is still buried.”
That is much more valuable than a vague promise about “AI scheduling.”
What We Think A Better Product Starts With
My guess is that better scheduling software starts with clarity.
Not with the biggest rules engine. Not with the broadest enterprise scope. Not with the most triumphant automation claim.
It starts by making the schedule easier to read, easier to trust, and easier to change without chaos.
If that turns out to be right, the deeper automation can come later. If it turns out to be wrong, we would rather learn that early.
If you want to pressure-test the idea against your actual workflow, book a demo. We will walk through the current direction, learn where the current process actually hurts, and decide what the first version should do.