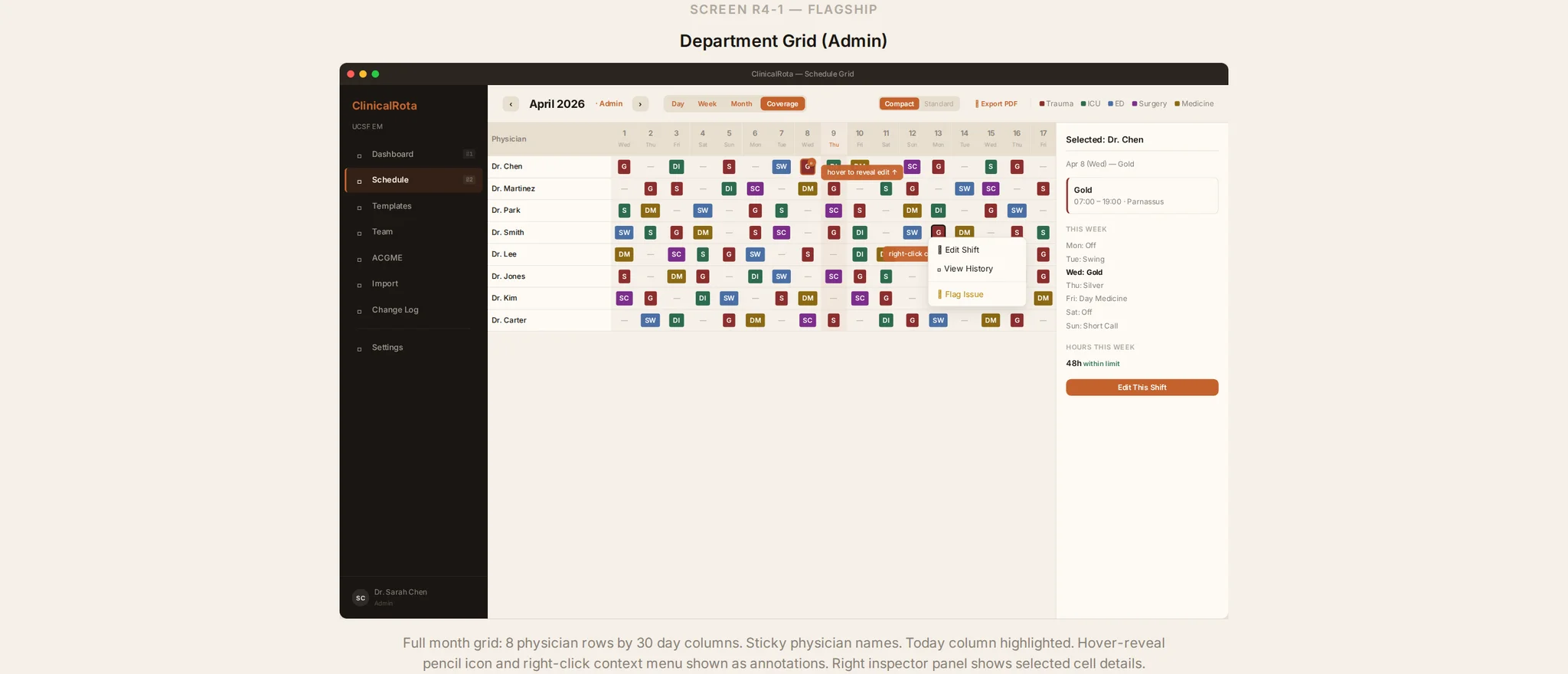
The Buffer That Keeps the Floor Running
Hospital scheduling systems are built around a baseline: the employed staff who fill the core schedule, the rotation rules that govern coverage, and the shift patterns that reflect how the unit is supposed to operate. Get the baseline right and the schedule mostly works.
But hospitals do not operate at baseline. Census fluctuates. Staff call in sick. A run of unplanned departures can leave a unit short for weeks while recruiting catches up. Winter brings respiratory illness. Summer brings vacation requests. The baseline schedule is the foundation, but the float pool is what keeps operations intact when something unexpected happens.
Float pool management is not a niche concern. For most acute care hospitals, supplemental staffing, including per diem employees, float pool nurses, and agency or travel staff, represents a meaningful portion of actual coverage on any given shift. Quality of care depends on having the right number of skilled, credentialed staff on the floor. Financial performance depends on not paying agency rates for coverage you could have filled from your pool. Operational performance depends on knowing, in advance, what your pool can actually deliver.
Most hospitals are managing this with tools that were not designed for it.
What Makes Float Pool Scheduling Different
The standard scheduling problem, assigning available staff to open shifts according to rules and preferences, is complicated enough with employed staff. Float pool scheduling adds layers that make standard tools a poor fit.
Availability is fluid and self-reported. Employed staff work a defined schedule with known availability. Per diem employees have no guaranteed hours and determine their own availability windows, often week to week or even day to day. A system built around predictable shift assignments struggles to capture this. Float pool coordinators end up maintaining a separate phone tree or text chain to canvass availability every time a gap appears.
Qualifications vary significantly within the pool. Not all per diem nurses are interchangeable. ICU float pool staff have different competencies and credentials than medical-surgical float pool staff. Some are certified in specialized monitoring; some have limited pediatric experience; some are cleared for certain high-acuity environments and not others. Placing a float pool nurse in a unit where they are not credentialed is not just inefficient, it is a patient safety risk. Manual tracking of who is cleared for what, and whether those credentials are current, is exactly the kind of task that gets missed when the schedule is being filled on short notice.
Agency staff add their own compliance layer. Agency and travel nurses come from outside the organization. They arrive with credentials from their agency, but the receiving hospital still has a responsibility to verify orientation completion, confirm that required competency assessments have been done, and track when those assessments expire. This documentation burden often falls on the nurse manager or unit coordinator, not on a centralized system, which means it is inconsistently done and hard to audit.
Cost visibility is fragmented. Per diem and agency staff are paid differently than employed staff. Agency rates are often significantly higher, which means every agency shift carries a premium cost. Managers who are trying to manage labor budgets need to know not just whether the schedule is covered but whether it is covered in a way that the budget can absorb. When scheduling and cost tracking live in separate systems, or when cost data only becomes visible after payroll runs, managers are making coverage decisions with incomplete information.
The Float Pool Coordinator’s Daily Reality
Float pool coordinators in acute care hospitals describe their role in terms that highlight the ad hoc nature of how supplemental staffing typically operates.
On any given morning, there are unfilled shifts across the facility, a list of float pool nurses whose availability they are trying to confirm by phone and text, a queue of last-minute sick calls from employed staff, and a set of unit managers who need to know by a certain time whether their shift will be covered. The coordinator is doing all of this in real time, drawing on memory and personal relationships with pool members as much as on any formal system.
This works until it does not. The failure modes are familiar: a nurse gets placed in a unit they were not fully oriented to because the coordinator did not have a quick way to check; a credential expires and no one notices until a nurse shows up for a shift they technically should not take; a unit ends up overstaffed because two people filled the same gap through different channels; an agency shift gets scheduled when a per diem nurse would have been available if someone had checked.
Each of these failures is individually recoverable. Taken together over a quarter, they create real cost in overtime, agency premium, preventable adverse events, and coordinator burnout.
What a Scheduling System Built for This Looks Like
A scheduling system designed to manage float pools and supplemental staffing handles the core complexity differently than a general-purpose scheduling tool adapted for the purpose.
Availability capture is structured. Per diem staff submit their availability through the system, which maintains a current record without requiring the coordinator to canvass by phone. Changes to availability update the pool’s coverage picture in real time. When a gap appears, the coordinator can filter for pool members who meet the placement criteria for that unit instead of working through a phone tree.
Credentials and placements are linked. The system tracks which pool members are cleared for which units, when unit-specific orientations were completed, and when recertifications are due. A placement recommendation only surfaces staff who are eligible for that unit. Expiring credentials trigger alerts before they become a problem at shift time. This is not a replacement for clinical judgment, but it eliminates the category of error where a well-intentioned placement goes wrong because the credential information was not in front of the person making the decision.
Agency integration is a documented workflow. When agency or travel staff are added to fill gaps the pool cannot cover, their onboarding and orientation records flow through the same system that manages employed and per diem staff. The receiving unit has a record of what assessments have been completed and what restrictions apply. Credential expiration tracking extends to agency staff, not just pool members.
Labor cost is visible at scheduling time. Coordinators and managers can see the cost differential between filling a shift from the per diem pool versus from an agency contract before confirming the placement. Budget consumption can be tracked against shift-level cost visibility rather than reconstructed from payroll data after the fact.
The Business Case Is About Margins and Risk
The argument for investing in purpose-built float pool scheduling is not primarily about coordinator productivity, though the efficiency gains are real. It is about the financial and quality risks that arise when supplemental staffing management is undisciplined.
Agency nursing is expensive. The premium over employed and per diem rates can be substantial, and it compounds quickly when agency shifts are being used because the float pool coordination process is not surfacing available pool members efficiently. Hospitals that improve float pool utilization by filling more shifts from the per diem pool before reaching for agency coverage often see a meaningful reduction in premium labor spend.
The quality and compliance risks are harder to quantify but not harder to understand. A nurse placed in a unit where their credentials were not current, or whose agency orientation was not documented, represents a risk that should not be accepted because the scheduling tool was not built to flag it.
Float pool management is, at its core, a data problem. The data exists: availability, credentials, placement history, cost rates, and orientation records. What is missing in most hospitals is a system that makes that data accessible at the moment a scheduling decision is being made.
If supplemental staffing complexity is creating cost and compliance risk in your department, book a demo to talk through your scheduling workflow and see where Clinical Rota fits today.