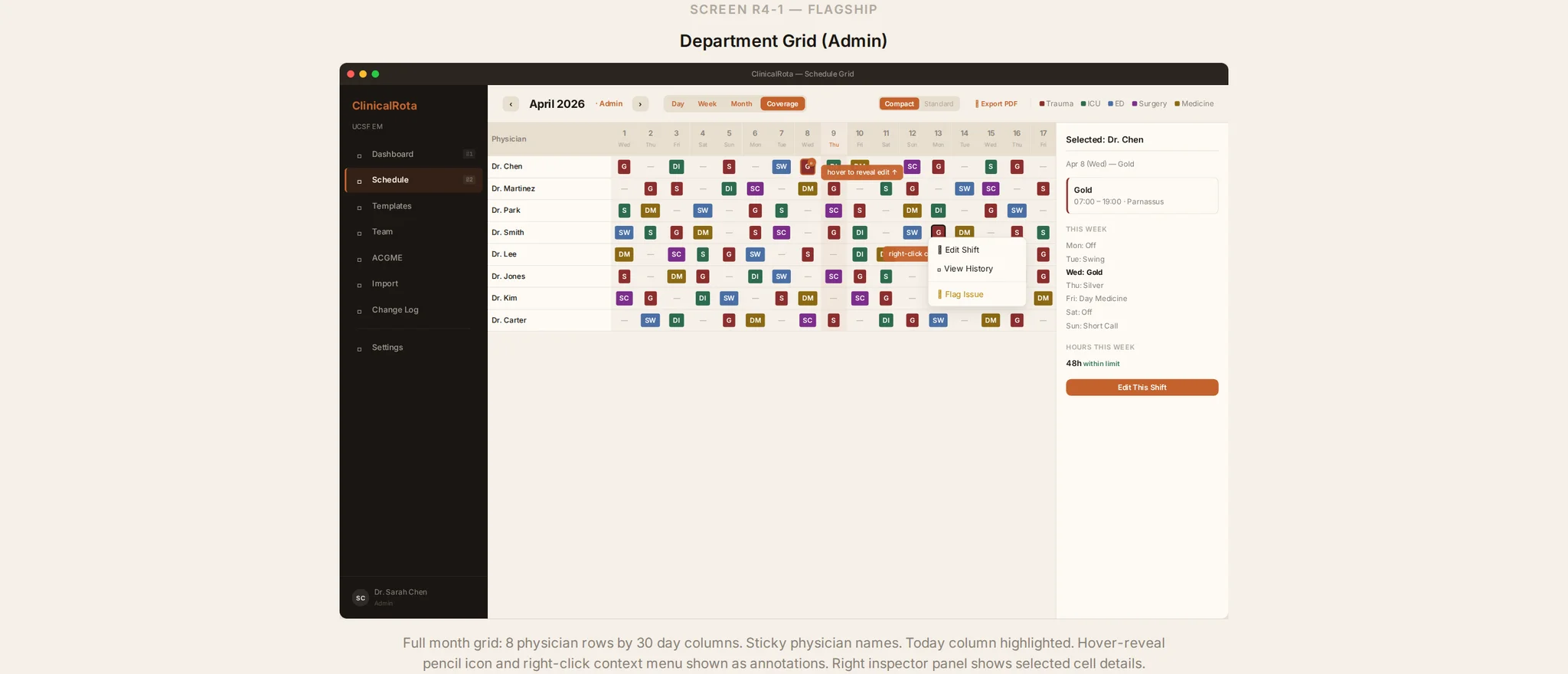
Why Emergency Medicine Is Different
Every hospital unit has scheduling complexity, but emergency departments combine the hardest parts of staffing into one environment. Demand is volatile, coverage gaps become urgent almost immediately, and the department has to remain fully operational around the clock.
Inpatient units deal with variable census, but staffing adjustments usually happen over hours, not minutes. Operating rooms work in blocks with more predictable durations. Even ICUs, despite their acuity, typically operate with steadier staffing ratios.
Emergency departments have fewer of those stabilizers. Patient volume can change sharply, shift handoffs occur on a fixed clock, and there is no safe option to close the unit or meaningfully slow intake. The department has to stay staffed regardless of whether the prior shift ran late or the next physician called out.
That is why scheduling failures in emergency medicine show up faster and more visibly than they do in most specialties. A gap in the physician schedule is rarely a problem for next week. It is often a problem for the next few hours.
The Structural Challenges
Volume Unpredictability
Emergency department volumes vary by day of week, time of day, season, and local epidemiology in ways that are partially predictable but never precise. A department that sees 250 visits on a slow Monday can easily see 380 on a Friday afternoon when respiratory illness is moving through the community.
Most scheduling tools treat coverage as binary: either a physician is on shift or they are not. ED scheduling needs a more operational view. Coverage has to track expected demand, and expected demand is a range, not a single number.
That means the schedule has to leave room for flexibility through overlap periods, backup call tiers, and a clear way to bring in help when the department surges. Those are not nice-to-haves. They are core design requirements.
Shift Pattern Complexity
Emergency medicine uses a wider mix of shift patterns than almost any other specialty. Eight-hour, ten-hour, and twelve-hour shifts often coexist with split shifts and deliberate overlap windows. In larger departments, attending coverage is commonly weighted toward the hours when demand is most likely to spike.
That variety creates real modeling problems. A system optimized for standard twelve-hour shifts will not reflect a department that uses six-to-six, seven-to-seven, and eight-to-eight patterns in the same schedule. Once shift templates vary across the group, the scheduling problem becomes materially harder.
Generic tools often respond by forcing those patterns into one template. The schedule may still look valid on paper, but it no longer reflects how the department actually runs.
Coverage Gaps Are Immediate Crises
In many specialties, a sick call creates a gap that has to be solved by tomorrow. In emergency medicine, a physician who calls in sick at 10 PM may need to be replaced by 11 PM.
That compresses the margin for error in schedule maintenance to almost nothing. The scheduler, often a chief resident, medical director, or ED administrator, needs a fast way to identify who is available and how to reach them. Spreadsheets and group texts are still common, but they are poor tools for a time-sensitive coverage problem.
Short-notice gaps are also a major source of unplanned overtime. Every premium dollar spent on last-minute coverage is a sign that the process failed earlier than it should have.
ACEP Wellness Guidelines
The American College of Emergency Physicians has published scheduling and wellness guidance that many departments now treat as a practical standard. It covers shift length, shift frequency, recovery time between shifts, and limits on consecutive overnight coverage.
Building a schedule that respects ACEP guidance while also meeting coverage needs and physician preferences is a legitimate optimization problem. Many ED schedulers are still doing that work manually, which turns the guidelines into soft constraints that slip when coverage pressure rises.
When that happens, the consequences are not abstract. Physicians working tighter turnarounds, carrying more overnight shifts than is advisable, or returning without adequate recovery time face a higher risk of burnout and adverse clinical events. The literature on fatigue and patient safety in emergency settings is clear on that point.1
Continuity and Handoff Quality
Emergency medicine has a different relationship with continuity than most specialties. In inpatient medicine, continuity often means the same attending follows the patient over several days. In the ED, continuity is more often about handoff quality between the physician leaving and the physician arriving.
Schedules that create handoff pressure can erode that process. When physicians are rushing out at shift end because the next team is not fully in place, the quality of the transition suffers. Adverse events in the ED cluster disproportionately around shift changes.2
Supporting a clean, unhurried handoff is therefore a real scheduling objective. It requires attention to where overlaps occur, how long they last, and whether that overlap is adequate for the acuity and patient mix typically present at that hour.
Where Standard Scheduling Tools Break Down
Generic scheduling tools, including many that were adapted for healthcare, were not designed around emergency medicine’s specific constraints. They tend to fail in predictable ways.
They don’t model demand-based coverage. Most tools ask whether a physician is assigned to a time slot. They do not ask whether that assignment is adequate for the expected volume. A department that regularly understaffs Friday evenings because the grid says the shift is covered is working from the wrong definition of coverage.
They can’t handle shift pattern variety. Tools designed around uniform twelve-hour shifts struggle with the mix of patterns that ED scheduling usually requires. The result is a patchwork of manual workarounds that strips away most of the value the software was supposed to provide.
They have no short-notice gap management. When someone calls in at 10 PM and another physician has to be on by 11 PM, the problem is not just scheduling. It is communication and availability. Most tools offer no real mechanism for that scenario, so the phone tree begins and the scramble starts.
They track compliance but don’t optimize for it. A tool that checks ACEP-related rules after the schedule is built can help with auditing. It does not help much if the goal is to build a schedule that avoids those problems in the first place.
What Better ED Scheduling Looks Like
Departments that move beyond generic tools and toward purpose-built scheduling usually improve in the same few areas.
Demand-informed coverage. Historical volume data can be layered into the coverage model so schedulers build demand-adjusted schedules instead of uniform ones. In practice, that means more physician time during predictable peaks and less excess coverage during reliably quiet periods.
Automated ACEP compliance checking. When wellness rules are enforced during schedule construction, violations are less likely to be introduced at all. The published schedule is closer to compliant by design, not compliant only after someone audits and revises it.
Short-notice gap management. A structured method for urgent coverage, such as an availability list, automated outreach, and a defined escalation path, turns a crisis into a process. Reaching a replacement in twenty minutes instead of ninety can be the difference between an orderly handoff and a genuine safety risk.
Fairness tracking over time. Emergency medicine has the same fairness dynamics as every other specialty. If the same physicians repeatedly absorb more overnights, holiday coverage, and surge-heavy shifts, resentment builds and retention suffers. Looking at distribution over quarters instead of a single schedule cycle helps leaders spot those patterns before they become staffing problems.3
The Stakes
Emergency departments are unforgiving environments for scheduling errors in either direction. Undercoverage increases safety risk and staff burnout. Overcoverage consumes scarce physician time and drives unnecessary labor cost.
Departments that get scheduling right benefit from better coverage, cleaner handoffs, stronger wellness compliance, and a fairer distribution of difficult shifts over time. Those operational advantages usually turn into retention advantages as well.
The dividing line is rarely intent. More often, it is whether the department has a process that matches the complexity of the work.
Clinical Rota is built for the realities of emergency medicine scheduling, including variable demand, urgent coverage gaps, and long-term fairness. Book a demo to see how it could work for your department.
References
Philibert, I. “Sleep loss and performance in residents and nonphysicians: a meta-analytic examination.” Sleep, 2005. Physician fatigue following inadequate rest periods is associated with increased medical error rates and adverse clinical outcomes, with emergency medicine identified as a high-risk specialty due to shift structure. ↩︎
Joint Commission Center for Transforming Healthcare. “Improving Transitions of Care: Hand-off Communications.” Research on adverse event clustering at shift transitions in high-acuity settings is consistent with Joint Commission findings on communication failures during care transitions. ↩︎
Shanafelt, T.D., et al. “Changes in Burnout and Satisfaction With Work-Life Integration in Physicians and the General US Working Population Between 2011 and 2020.” Mayo Clinic Proceedings, 2022. Organizational justice, including fair workload distribution, is a significant independent predictor of burnout across specialties, with emergency medicine reporting among the highest burnout rates. ↩︎